Using birth control isn’t only about preventing pregnancy. Birth control is a critical tool for women’s health care and sexually transmitted disease (STD) control. Luckily, there are so many forms of birth control to choose from, which sometimes can feel overwhelming when trying to find the right one for you. That’s why we’ve done the hard work for you, and outlined all your options below!
Some birth control methods may work better than others depending on your medical history, lifestyle, if you want children now or in the future, and your need to prevent sexually transmitted infections.
In the United States, there are over a dozen contraceptive methods and options available to choose from – which is a lot! They range from long-lasting reversible contraceptives, such as intrauterine devices (IUDs), to shorter-term methods, like the pill, patch, or ring –which predominantly rely on hormones to prevent pregnancy. There are also non hormonal options like condoms or the copper IUD. So what is the difference between hormonal and non hormonal birth control? Why use one over the other? Can you use these methods together? Consider this your hormonal vs. non-hormonal crash course in birth control –knowledge is power!
What is Hormonal birth control and How Does it Work?
Hormonal birth control uses hormones in a safe and effective way to prevent pregnancy. All hormonal contraceptives contain progesterone or a combination of progesterone and estrogen. The two hormones work together to prevent pregnancy by blocking ovulation (i.e. the release of an egg), thinning the lining of the uterus (a.k.a endometrium), and thickening the cervical mucus plug to prevent sperm from entering the uterus. Progestin only pills (POPs) or mini-pills work by thickening the cervical mucus to block sperm from reaching the egg and thinning the lining of the uterus. 40% of those with uteri will still ovulate on traditional POPs.
Types of Hormonal Birth Control
With hormonal birth control you have a wide range of options to choose, from the most effective to the least effective:
-
- Birth Control Implant
- Birth control IUD
- Birth control injection
- Birth Control ring
- Birth control patch
- Birth control pill
Birth Control Implant
The hormonal implant (Nexplanon) is the most effective birth control option for preventing pregnancy, beating vasectomy! It’s a very small rod (the size of a matchstick) that is inserted under the skin of the upper arm and prevents pregnancy for up to 5 years. Like the hormonal IUD, the implant releases small, continuous amounts of progestin (specifically, etonogestrel) over its life to prevent pregnancy and is 99% effective (on average only 1/1000 people using it will get pregnant).
Because it is implanted under the skin, a doctor’s office visit is required for insertion and removal.
Hormonal IUD
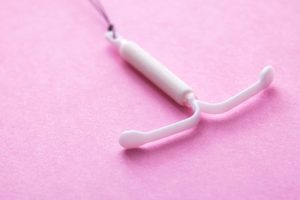
The hormonal IUD is a T-shaped, flexible plastic device that is inserted into the uterus by a doctor or other trained health professional. It works by releasing a small, steady dose of hormones over time.
Hormonal IUDs (Mirena, Liletta, Kyleena, Skyla) release the progestin levonorgestrel, which keeps the uterus lining thin so it can’t support a pregnancy and causes the cervical mucus to be thick to block the sperm. They are 99% effective in preventing pregnancy and last 3-8 years depending on the type. The fewer the years, the more likely you will have monthly bleeding with that option.
Birth Control Injection
The shot, also known as Depo-Provera, is a low-maintenance, highly effective form of longer-term birth control that is injected every 12 weeks.
The birth control shot contains the hormone, progesterone acetate, which helps prevent pregnancy by preventing ovulation. It also thickens the cervical mucus to prevent sperm from getting to the ova (eggs that are released each month). It is 96% effective at preventing pregnancy and can either be self administered or done via doctor’s appointment.
Birth Control Vaginal Ring
The vaginal ring is a small, flexible silicone ring placed inside the vagina that prevents pregnancy as it releases a continuous dose of hormones (etonogestrel and ethinyl estradiol). The ring is 99% effective with perfect use and 93% effective in typical use.
Depending on the brand, the ring can last 35 days (NuvaRing, Eluying) or 1 year (Annovera). Rings are generally left in for 21-24 days, and then removed for 7 or 4 days and replaced with a new ring (monthly ring) or reinserted (one year ring). Many consider the contraceptive vaginal ring to be more convenient than the pill because you only have to change it out once every three weeks, monthly, or once a year!
You can leave the birth control ring in during sexual intercourse. You can also take it out and leave it out for up to 3 hrs but make sure you put it back in or you risk pregnancy.
Patch
Much like the vaginal ring, the birth control patch is just as effective at preventing pregnancy – it just requires weekly replacement, which you easily do yourself. The birth control patch contains the same types of hormones as the combination pill and vaginal ring: progestin and estrogen. The patch is 99% effective when used perfectly and 93% in typical use.
It is important to note that both the Xulane and Twirla patches have a BMI limitation of 35. Those with a BMI over 35 should not use the birth control patch because it has a higher risk of blood clots and lower efficacy in those with a BMI of 35 or more.
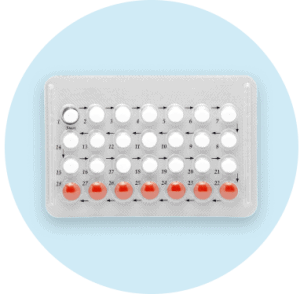
Pill
There are two types of birth control pills: the combined oral contraceptive pill (which contains both estrogen and progestin) or the progestin-only pill (POP) a.k.a the “mini-pill.” Pandia Health offers over 135 different birth control pills to choose from and it can be hard to know where to start. Luckily you can use our expert birth control doctors to match you with your perfect fit.
The pill works by stopping sperm from fertilizing an egg. The hormones in the combined birth control pill stop ovulation, meaning there’s no egg for the sperm to fertilize. Progestins in the pill thicken the mucus in the cervix, making it harder for a sperm to swim to an egg. Progestins also thin the lining of the uterus, resulting in less blood loss with withdrawal bleeds. When used perfectly (taken at the same time everyday), the pill is 99% effective at preventing pregnancy.
Benefits of Hormonal Birth Control
In addition to pregnancy prevention, hormonal birth control has several other benefits. It can help reduce the chance of developing certain reproductive issues and cancers, ease painful periods, help treat acne, and more.
Preventing Ovarian Cysts or Cancer
Taking hormonal birth control, such as the pill, patch, ring, or IUD, can be an effective method in preventing ovarian cysts from forming. While cysts cannot be entirely prevented, an individual may be able to decrease their risk of developing one if they take hormonal birth control. Because ovarian cysts form during the process of ovulation, preventing ovulation can reduce the likelihood that a cyst will form. Using the birth control pill, patch, or ring for 5 years decreases your risk of ovarian cancer by 50%.
Making #PeriodsOptional
If you use the birth control pill, patch, or vaginal ring, you can easily skip your period for up to 3 months or more –and it’s safe to do so! If you’re on the pill, skipping your period is as easy as skipping the placebo week and starting the next pack! If you’re on the ring, it’s as easy as skipping the ring-free week (you can change the ring once a month or every 28 days, your choice). With the patch you can skip up to 12 weeks in a row at a time but then you must stop for 1 week (After that, the estrogen from the patch builds up and increases your risk of blood clots). Learn more about #PeriodsOptional and its benefits on the linked page.
Treat period problems a.k.a painful periods
The birth control pill, patch, and ring make your periods regular and easy to predict. The hormones in the pill, patch, ring also help reduce menstrual cramps and reduce heavy flow, making your periods lighter, less painful and less uncomfortable.
Acne
Acne is a direct result of an imbalance of the hormones: estrogen and testosterone. It is the excess of testosterone that can lead to acne. Fortunately, birth control pills, patches, and rings decrease the amount of testosterone being made or the amount of testosterone running around in the blood, preventing the excess of “male” hormones in your system. More specifically, being on the pill, patch, or ring increases the sex hormone binding globulin, a protein that binds to the extra testosterone, resulting in less of it being around.
[thrive_leads id=’20040′]
Downside of Hormonal Birth control
Hormonal birth control methods are among the safest and most effective methods of contraception. However, some people may experience side effects. Side effects can include nausea, breast tenderness, mood changes, spotting, and headaches.
If you are on an estrogen-containing method, taking hormonal birth control may increase an individual’s risk of developing blood clots. The hormones in the combination pill, patch, and ring (especially estrogen) can affect blood clotting factors. With that being said, the overall risk of getting blood clots when taking hormonal birth control is very small (3/1000 to 1/100 if you take the pill for 10 years).
People with uteri who have family or personal history of blood clots, migraine with aura or are over age 35 and smoke have a much higher risk of developing blood clots while taking hormonal birth control. If you have these health issues, doctors will only provide a type of contraception that does not contain estrogen, such as the IUD or progestin-only (mini) pill.
The risk of serious side effects is very low if you are under 35 years old and a nonsmoker.
Hormonal methods of birth control do not offer protection against STIs.
What is non hormonal birth control
Simply put, non hormonal birth control is birth control options that prevent pregnancy and do not use hormones.
A benefit of non hormonal birth control is that it avoids changes in hormone levels.There are multiple different non hormonal birth control methods that work in different ways. The copper IUD does not have hormones and works by being toxic to sperm and ova (egg). Barrier methods like condoms or the diaphragm work by preventing sperm from reaching the egg. Phexxi is a vaginal gel that works by making it hard for the sperm to move. Fertility awareness methods and apps (applications) work by telling you when NOT to have sex to decrease your risk of getting pregnant.
Those who have medical conditions such as chronic migraines with aura, high blood pressure, or risk of blood clots will most likely have to use non hormonal methods vs hormonal methods of birth control because of the risk of blood clots.
Types of Non Hormonal birth control types
There are many non hormonal options for those looking to effectively prevent pregnancy.
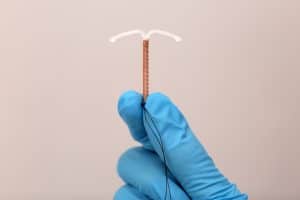
Copper IUDs
Copper IUDs (Paraguard) are T-shaped, flexible, made of plastic, wrapped in copper. It is a non-hormonal birth control option and works by making a very ‘hostile’ environment for sperm and ova(eggs). The copper IUD is very effective at 99% and works up to 12 years. Copper IUDs require insertion by a medical professional. A side effect of this option may be very heavy periods and stronger cramps.
Barrier methods (condoms, diaphragm, cervical cap, the contraceptive sponge) work by establishing a physical barrier between the egg and the sperm to prevent pregnancy, but they are also less effective than hormonal birth control methods.
Condoms
Male condoms and female condoms are the most common barrier methods and the only birth control option that also works to prevent sexually transmitted infections. In everyday use, condoms are 87% effective in preventing pregnancy. This method is typically used with another method, for a higher efficacy rate.
Diaphragm
A diaphragm is a reusable silicone cup, inserted with spermicide by the user into the vagina to cover the cervix. Diaphragms can be inserted up to 2 hours before sex; any longer and the spermicide won’t be as effective. Diaphragms should be left in for at least 6 hours after sex, but no longer than 24 hours. The diaphragm should NOT be removed if you have sex again within 6 hrs. You should wait for 6 hrs after the last ejaculation to remove the diaphragm. If the diaphragm has been in place for more than 3 hrs, you need to add more spermicide to the outside. When used consistently and correctly, diaphragms are 84% effective at preventing pregnancy, but due to the complexity of use, they are not a very popular option.
Cervical Cap
A cervical cap is a reusable small silicone cap inserted by the user inside the vagina to block sperm from reaching an egg. Like the diaphragm, it covers the cervix and should be left in for at least 6 hours after sex. A cervical cap should not be left in for longer than 48 hours. Cervical caps are about 86% effective. Cervical caps require a prescription from a doctor and can last up to a year if taken care of properly.
Contraceptive Sponge
The contraceptive sponge (discontinued) is a barrier method made of foam with spermicide inside. Similar to a cervical cap and diaphragm it is inserted into the vagina and used to block sperm from reaching an egg. When used correctly the sponge is about 80% effective in preventing pregnancy if you have had a baby before and 91% if you have not had a baby before. The sponge should be left in for 6 hours after sex and removed within 30 hours of insertion. Sponges are not reusable and should be thrown away after use. The sponge can be bought over the counter without a prescription and already contains spermicide. Sponges are not a popular option because they are often used incorrectly, reducing effectiveness.
Spermicide
Spermicide is a chemical used to paralyze and kill sperm inside the vagina. Spermicide is sold in the form of gels, foams, creams, and suppositories. Spermicide can be and is recommended to be used alongside other barrier methods to boost effectiveness. Used alone, spermicide is about 79% effective in preventing pregnancy. Used with condoms, using both spermicides and condoms at the same time has a 97% efficacy in preventing pregnancy.
Benefits of Non Hormonal birth control
Many people choose to take non hormonal birth control to avoid the possible side effects that might happen hormonal birth control,especially those with medical conditions that might have higher risk of blood clots.
Pre-existing medical conditions or other health problems like high blood pressure, smoking, and a family history of breast cancer are important factors for you and your doctor to consider when choosing the best birth control method for you. Some birth control options have side effects that may not be present in other methods. For example, if you get headaches while taking the pill or are at risk for blood clots, a non hormonal method of birth control may be best for you.
Downsides of NonHormonal birth control
Non hormonal birth control is generally not as effective as hormonal birth control except for the copper IUD which beats most methods except vasectomy, implant, hormonal IUD, and tubal ligation. Considering many non hormonal methods are barrier methods, knowing how to properly use non hormonal methods is crucial to their effectiveness.
Additionally, methods such as diaphragm and cervical caps can be uncomfortable to put in your vagina compared to hormonal methods such as the pill or patch.
Although copper IUDs are highly effective, know that the most common side effects are more bleeding and more cramps during your periods.
Which one is right for me?
So, what’s the verdict? Would you prefer hormonal or non hormonal birth control when looking for a contraception method? For more than 70 years, hormonal contraceptives have been studied extensively and found to be safe for most women. However, like any medication or health choice, it’s important to see a doctor, weigh the risks and benefits for you specifically, and make an informed decision about which method of birth control is right for you.
Beyond obvious health risks, if you are nervous about hormonal birth control because of fear of the impact that hormones will have on your body –you can rest easy knowing that there is no scientific evidence that shows long term health risks associated with hormonal contraception other than slight increase risk of breast cancer. This risk is less than the risk of breast cancer from drinking 3-6 glasses of alcohol a week.
If you’re still on the fence about which type is right for you, our expert birth control doctors will help you navigate this journey. Or, to automate your birth control (get it delivered!), Pandia Health is the place for you! Our online platform makes it easy to get started with our service.
Disclaimer: This article, even if and to the extent that features the advice of physicians and medical practitioners, it is not, nor is it intended to be, a substitute for professional medical advice, diagnosis or treatment, and should never be relied upon for specific medical advice. Always seek the advice of your doctor/primary care provider for specific health needs.