Medically reviewed by Catherine Hansen, MD, OBGYN & Menopause specialist
Can you get pregnant after menopause? Directly speaking, natural pregnancy is highly unlikely once you enter menopause. In this article, we’ll explain why this is the case, the role hormones play, and what options exist for motherhood beyond the menopausal threshold.

Understanding Menopause and Its Stages
Menopause, the natural conclusion of a woman’s reproductive years, typically unfolds between the ages of 45 and 55. It’s a gradual process that doesn’t happen overnight but rather progresses through several stages, each marked by significant hormonal shifts and changes in fertility.
We’ll navigate through these stages, examining the intricacies of perimenopause, the conclusiveness of menopause, and the lifestyle in the postmenopausal stage. Along the way, we’ll delve into the impacts of hormonal changes, the cessation of menstrual cycles, and answer that intriguing question— can a woman conceive after menopause?
Perimenopause
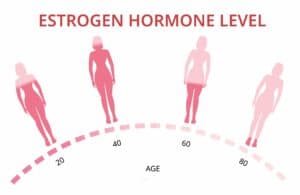
Perimenopause is the prologue to menopause, often called the menopausal transition, where a symphony of hormonal changes begins. This stage can start as early as the late 30s to 40s and is characterized by a notable decline in estrogen and progesterone, alongside an increase in LH and FSH levels. These hormonal fluctuations can lead to a host of symptoms such as hot flashes, night sweats, mood changes, and notably, irregular menstrual periods.
Despite the erratic nature of the menstrual cycle during this time, conception remains a possibility. However, fertility starts to wane as the ovarian reserve dwindles, and ovulation becomes less predictable. This phase demands increased consciousness for women who might still desire to conceive or for those who choose to avoid pregnancy.
Menopause
Menopause is not just an event but a diagnosis confirmed after a woman has gone 12 consecutive months without a menstrual period. It heralds the end of natural fertility, as the ovaries stop releasing eggs, and hormone levels, particularly estrogen and progesterone, stabilize at lower concentrations. This woman’s life stage typically occurs between 40 and 55 years of age, with 51 being the average.
The decreased estrogen levels after menopause bring about various bodily changes, from increased fat storage to vaginal dryness. While these shifts signal the end of one’s ability to conceive naturally, they also usher in a new phase of health considerations.
Postmenopause
Postmenopause is the chapter following the final menstrual period. For some, it may continue to echo the menopausal symptoms experienced earlier. However, it is also a period of adaptation to new hormone levels and an increased focus on maintaining health to mitigate risks such as heart disease and osteoporosis.
Fertility Decline with Age: The Impact on Pregnancy
As the candles on the birthday cake multiply, fertility quietly begins its retreat. This decline starts subtly around age 32 and accelerates after age 37, affecting pregnancy rates and increasing the likelihood of fertility-related disorders. For women, this ticking biological clock signals a changing landscape in their reproductive capabilities.
The decline in fertility is not just about the number of eggs but also their quality. As a woman ages, her ovarian reserve diminishes, and the chromosomal integrity of oocytes can be compromised, leading to potential genetic abnormalities and presenting challenges for natural conception and the success of fertility treatments.
Ovarian Reserve and Aging
Ovarian reserve is a term that refers to the pool of eggs nestled within a woman’s ovaries. From a peak of several million while growing in your mother’s womb, this reserve spirals to a mere thousand by menopause. The decline in ovarian reserve is a natural process, yet can be hastened by lifestyle choices such as smoking, medical conditions like severe endometriosis or genetics.
Genetics also play a role in how quickly one’s ovarian reserve depletes, particularly if there’s a family history of early menopause. And as the reserve wanes, so does the quality of the eggs, which can lead to spontaneous abortions or genetic disorders in offspring due to chromosomal abnormalities.
Hormonal Changes and Their Effects
The hormonal changes that accompany aging are like a domino effect impacting fertility. Early rises in follicle-stimulating hormone (FSH) herald the beginning of ovarian aging and a reduction in anti-Müllerian hormone (AMH). These hormonal shifts signal a decline in fertility, making natural conception difficult and reduce the success of fertility treatments.
For perimenopausal women, these hormonal changes mean a dwindling number of eggs and age-related uterine changes, which complicate pregnancy. While these changes are a natural part of aging, they can have significant effects on a woman’s ability to conceive naturally.
There have been extensive advances in fertility care and it may be possible, through interventions such as in vitro fertilization (IVF) using donor embryos or donor oocytes (eggs) to conceive a healthy pregnancy and gestational carriers or surrogates are also a possibility that is gaining favor.
Can You Conceive Naturally After Menopause?
The question of whether one can conceive naturally post-menopause is akin to asking if a garden can bloom without water. Once menopause has been confirmed, and a woman has gone a full year without a period, the natural reproductive years are considered over. The cessation of ovulation and menstruation signals an end to the possibility of getting pregnant naturally, thus eliminating the chance of a natural pregnancy.
However, the question isn’t just about the biological possibility but also about the realities of life post-menopause. It’s a time when the body settles into new patterns, and hormone levels are no longer conducive to ovulation or supporting a natural pregnancy. The idea of trying to get pregnant after menopause, then, becomes more of a theoretical discussion than a practical one. If this is a serious consideration for you, consult with a fertility clinic and speak with a reproductive endocrinologist who will be able to advise about the most up-to-date options.
Menstrual Cycle Cessation
The end of the menstrual cycle marks a defining moment in a woman’s life. Menopause is diagnosed after a year without menstruation, signifying the permanent end of the menstrual cycle and natural fertility. The number of oocytes, or eggs, decreases significantly, with about 1,000 remaining at the onset of menopause.
This cessation of menstruation is not just a sign of fertility ending but also a shift to a new phase of life. It’s a reminder of the natural progression of aging and a woman’s transition from the reproductive years to the postmenopausal period. It’s also the beginning of many amazing life experiences and new possibilities that are marked by maturity, wisdom and a whole new perspective on what’s important for health and happiness.
Health Risks for Older Mothers
For those who do become pregnant later in life, the journey is not without its challenges. Older mothers face increased health risks such as placental disorders (placenta previa, placental insufficiency, subchorionic hemorrhage) gestational diabetes and preeclampsia. The chances of miscarriage and genetic disorders in the offspring also rise with maternal age.
Despite these risks, acknowledging that expert fertility counseling and medical supervision can lead many women of advanced age to successful and healthy pregnancies. Modern medicine has opened the door to many possibilities for couples who would otherwise be left without children. Adoption is also a very viable and heart-centered option for couples who are looking to expand their family without the potential complications or risks of pregnancy.
Assisted Reproductive Technology: A Solution for Postmenopausal Women?
When the natural wellspring of fertility dries up post-menopause, modern science offers a reservoir of hope. Assisted reproductive technology, such as in vitro fertilization (IVF), can enable postmenopausal women to conceive, essentially bypassing the natural limitations imposed by menopause.
Owing to these progressive techniques, the termination of menstrual cycles doesn’t essentially signify the end of aspirations for motherhood. With options like frozen or donor eggs, postmenopausal women can embark on the path to pregnancy, a journey once thought impossible for this stage of life. In fact, many young, single women who are concerned will have a consultation to discuss egg freezing (oocyte cryopreservation) which should be completed as soon as possible to ensure young, healthy eggs are in reserve for a future pregnancy when timing is more appropriate.
Navigating Pregnancy During Perimenopause
Perimenopause represents a transitional phase, where conceiving continues to be a possibility despite diminished fertility. It’s a phase that requires effective birth control to prevent unintended pregnancies and an awareness of the potential health risks associated with conceiving during this stage.
Women in their perimenopausal years must navigate this time with care, considering the likelihood of pregnancy and the need for personalized clinical management to mitigate any risks.
Birth Control for Perimenopausal Women
Birth control remains a critical consideration for perimenopausal women. Despite the onset of irregular periods, the possibility of an unplanned pregnancy is higher compared to younger women. Thus, effective contraception is essential.
Safer birth control options for women over 40 include:
- Condoms
- Birth control pills: depending on your health history and needs you will have combined oral pill or the mini pill which contains only progesterone
- Birth control patch or ring
- Intrauterine devices (IUDs)
- Vasectomy for partners
Health Risks and Complications
Pregnancy during perimenopause carries increased risks, such as placental complications, miscarriage and gestational diabetes.
Understanding the unique risks associated with spontaneous conceptions during perimenopause, is key to ensuring the health of both mother and child.
Pandia Health: Your Partner in Menopausal Care
At Pandia Health, experts in hormonal care we are just a click away. If you want to be sure to be protected against pregnancy during perimenopause, our doctors can prescribe birth control to you from the comfort of your home. If what you are looking for is menopausal treatment to ease symptoms, we have doctors Menopause Society Certified Practitioners that stand at the forefront of personalized hormonal health.
Whether you’re in search of FDA-approved, bioidentical hormone treatment plans, educational resources, or online consultations for birth control, Pandia Health offers a holistic service customized for women navigating all stages of menopause. With the convenience of free delivery for your prescriptions, Pandia Health ensures that your journey through menopause is supported every step of the way. If you’re ready to say bye to menopause symptoms or need that but also want to be protected against pregnancy, start a consultation today!
Takeaway
As we wrap up our exploration of menopause and the reality of pregnancy during this phase of life, it’s clear that while the natural ability to conceive wanes with the transition into menopause, the dream of motherhood need not dim. Through the marvels of assisted reproductive technology and the guidance of health care professionals, even postmenopausal women have options to explore pregnancy.
Our journey from understanding the stages of menopause to recognizing the impact of aging on fertility, and the potential for conception through modern medicine, underscores the importance of informed health choices. May this guide serve as a beacon for all women navigating these waters, illuminating the possibilities and care available at each turn.