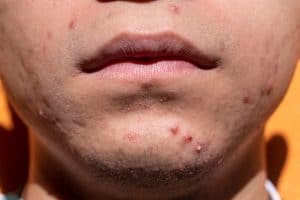
Noticing more facial blemishes than usual? Or little bumps on your face and body that just won’t go away? You might have fallen prey to a particular type of skin condition – fungal acne. While this may sound intimidating, it is both normal and treatable.

What is fungal acne?
Fungal acne is not really acne (blockage of the pores by sebum and bacteria and with inflammation). Fungal acne is actually a fungal infection of the hair follicle by malassezia (used to be called pityrosporum) that looks like regular acne (acne vulgaris). While often mistaken for regular acne, the cause is different.
Sebaceous or “oil” glands naturally keep our skin protected against friction and make the skin more impervious to moisture. Acne happens when your pores (Hair follicles) are blocked with dead skin cells, sebum(oil) and then can become pustules and/or have inflammation.
In contrast, fungal acne (fungal folliculitis) is an overgrowth of yeast within the hair follicles. When there is yeast in the sebaceous glands, your hair follicles become inflamed, causing “fungal acne.” Let’s explore what that can look like.
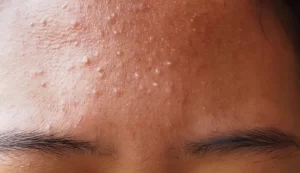
What does fungal acne look like?
Fungal acne can be often confused with a typical whitehead or acne papule. The lesions are usually grouped together with white bumps or pustules or red bumps (papules) of very similar size from 1-2mm.
Fungal acne (Malassezia folliculitis) can happen anywhere on the body but most commonly appears on the forehead, temples, hairline, upper chest, and mid-back.
Versus regular acne which comes in a variety of forms and sizes from: papules, pustules, blackheads, whiteheads, nodules (big painful bumps), cysts.
The bumps can get worse with:
- Very greasy skin
- Sweat
- Over-moisturizing, using too much sunblock, make-up which blocks your pores
being in a humid climate can increase your likelihood of developing fungal acne, because yeast thrives in this type of environment. - Tight fitting clothes with sweat, blocking the pores, increasing fungus growth
- Using antibiotics which kills bacteria but sometimes can result in fungus growing
Fungal Acne Vs. Regular Acne
Although regular acne and fungal acne have some similarities, there are several ways you can try to tell them apart.
How fungal acne feels vs. regular acne
Fungal acne: itching and burning
Regular acne: neutral to varying degrees of discomfort. Cysts can be very painful, large and scarring.
How fungal acne looks vs. regular acne
Fungal acne: white bumps with red skin surrounding them; bumps are uniform in size and usually occur in clusters.
Regular acne: varying appearances and sizes with any combination of whiteheads, blackheads, skin-colored bumps or cysts depending on the person; blemishes are more spaced out.
Where fungal acne is located vs regular acne
Fungal acne: can happen anywhere on the body but most commonly appears on the forehead, temples, hairline, upper chest, and mid back.
Regular acne: anywhere on your face (forehead acne, nose, acne on cheeks, chin acne, acne on jawline, hairline, temples), neck, acne on chest, or acne on back.
What causes fungal acne vs regular acne
Fungal Acne: fungus. Specifically Malassezia (used to be called Pityrosporum). (yeast)
Regular Acne: bacteria
How fungal acne is treated vs. regular acne
Fungal acne: You can try: bentonite clay masks, chemical exfoliants (lactic/salicylic acid), dandruff body wash, natural antifungals (oil of oregano, clove, walnut), more frequent showering, and looser clothes. What doctors will prescribe to treat your fungal acne aka fungal folliculities: antifungal creams or medications.
Regular acne: treatment of hormonal imbalances with birth control pill, patch, or vaginal ring, salicylic acid, topical retinoids, topical antibiotics, oral antibiotics, and/or oral retinoids.
What causes fungal acne on your face?
Fungal acne appears on your face due to yeast overgrowth, which may be due to trapped moisture, more moisture, a suppressed immune system, tight clothes, or humid environments. While having some fungus and bacteria on your skin is normal, an imbalance can lead to an overgrowth of yeast. Yeast can then enter into the sebaceous glands via the hair follicle and cause the inflammation and itchiness that comes with fungal acne.
How is fungal acne diagnosed?
Before treating fungal acne, consult a doctor to make sure that you do not have another skin condition. Even if fungal acne is suspected, a doctor or dermatologist may want to conduct a fungal test (skin scraping and look under the microscope) to diagnose fungal acne aka fungal folliculitis other causes before prescribing treatment.
Although you may want to jump into treatment as soon as possible, consulting a doctor is always best. Misdiagnosing your fungal acne could lead to ineffective treatment. For instance, if you start oral antibiotics to treat your fungal “acne,” if it turns out you have fungal acne due to a disruption of normal bacteria, the antibiotics could make your fungal acne worse.
How is fungal acne on the face treated?
Oral antifungal medication
Oral antifungal medication works by either directly killing or preventing the growth of fungal cells. Azoles are the most commonly used because they interfere with enzymes that help create the fungal cell membrane. This type of medication is taken by mouth as prescribed by your doctor. The benefit of oral acne medication is that it is fast and most effective.
Prescription topical anti fungal creams
If over-the-counter products do not improve your fungal acne, your doctor may recommend a more potent topical medication. Ketoconazole 2% is commonly prescribed, which is applied twice a day for 2 to 3 weeks to help reduce the overgrowth of yeast on the skin, which should get rid of the fungal acne a.k.a fungal folliculitis. However, whatever caused the fungal acne could make it come back again.
Diet adjustments
An antifungal diet involves reducing the intake of foods that promote yeast growth, such as refined sugar and white flour. While it’s not necessary to completely eliminate these food groups from your diet, finding a balance with other whole foods such as fruits, vegetables, grains, and lean meats could make a difference to your skin.
Antifungal shampoo or body wash
Antifungal shampoo and body wash can help slow down the growth of the fungi that cause infection. Most products can be purchased over-the-counter (selsun blue), but some may require a prescription from a doctor. They are applied to the affected area and rinsed off immediately or after a few minutes. While these products can be very effective, they can lead to side effects if you use them too often such as skin irritation. These can also be used to prevent the fungal acne from coming back.
Oil-free moisturizer
Oil-free moisturizers are great products as they provide moisture to the skin without introducing more oil that could get trapped by hair follicles. These can be purchased over-the-counter and applied as part of your daily skincare routine.
What’s the takeaway?
Fungal acne is not really acne and is actually a fungal infection or folliculitis that is caused by extra yeast growing in your hair follicle. While it may initially be mistaken for your typical blemish, acne should ideally be looked at by a doctor, who can help determine the appropriate treatment.
Thankfully, fungal acne is treatable and will likely go away within a short time with proper treatment.
You do not need to feel ashamed or embarrassed if you suddenly notice these irritating small bumps. Sometimes they are simply caused by living your life, and the best thing you can do is consult a doctor.
Disclaimer: The above information is for general informational purposes only and is NOT a substitute for professional medical advice. Always seek the advice of your doctor/primary care provider before starting or changing treatment.